Salt, the one we put on food, is composed almost exclusively of sodium chloride (NaCl) that very easily dissolves in water into positively charged sodium (Na+) and negatively charged chloride (Cl-) ions. And there is something very special and unique about these ions: in our blood, Na+ and Cl- are present in the highest concentrations and maintained in the narrowest of ranges. This is very revealing, and means, quite plainly, that sodium and chloride are the most important extracellular electrolytes. This is a simple fact. Now, forget everything you’ve heard, been told, or read about salt being bad for you, and consider this:
Our blood is made of red blood cells (45%) and white blood cells and platelets (0.7%) floating in blood plasma (54.3%). Blood plasma shuttles nutrients to cells around the body and transports wastes out. It consists of 92% water, 8% specialised mostly transporter proteins, and trace amounts of solutes (things dissolved or floating in it). And although circulating in trace amounts, the solutes—especially sodium—are vital. The concentration of solutes in blood plasma is around 300 mmol/l (don’t worry about the units for now). In the highest concentration of all is sodium at 140 mmol/l. In the second highest concentration of all is chloride at 100 mmol/l. The sum of these is 240 mmol/l. So, from these numbers alone, we see that blood plasma is more or less just salty water.

Pure alkaline water
Don’t you find this amazing? Don’t you find it amazing that nobody has ever told you this straight out in this way? And isn’t it amazing that we have been and continue to be told to avoid eating salt because it is bad for us: that it causes hypertension that predisposes us to heart disease? It really is completely amazing and ridiculous and also rather sad. But misunderstandings of this kind are unfortunately much more common than they should, as you may remember from What about cholesterol and Six eggs per day for six days: cholesterol?, but also from Minerals and bones, calcium and heart attacks and A diabetic’s meal on Air France. As you will understand for yourself in a few moments, the problem is not too much salt; the problem is not enough water:
Hypertension is not caused by excessive salt consumption. It is caused primarily by chronic dehydration, magnesium deficiency, and calcification.
Taking a look at the other electrolytes, bicarbonate (HCO3-), the primary pH regulator, is the third most highly concentrated molecule in plasma at 20 mmol/l. Potassium (K+) is the fourth at 4-5 mmol/l, then calcium (Ca 2+) and magnesium (Mg 2+) both at about 1 mmol/l. Therefore, the concentration of sodium in the blood is 7 times higher than that of bicarbonate, 40 times higher than that of potassium, and about 140 times higher than that of calcium and magnesium. And as with everything else in our body’s exquisite physiology, there are very good reasons for this:
Every cell in every tissue and in every organ of our body relies on an electrical potential difference between the fluid inside the cell membrane and the fluid outside of it in order to function: produce energy and transport things in and out. This is particularly important in active “electrical” tissues such as muscles and nerves, including neurones, that simply cannot work—cannot contract and relax in the case of muscle fibres, and cannot fire off electrical pulses in the case of nerve fibres and neurones—without a well-maintained and stable potential across the cellular membrane.
This resting potential across the membrane results from the delicate balance of the equilibrium potential and relative permeability through the cellular membrane of the three most important ions: Na+, K+ and Cl-. The potential is maintained by the sodium-potassium pump: a specialised protein structure in the membrane that ensures the concentration of potassium (K+) stays low outside the cell and high inside the cell, and conversely, the concentration of sodium (Na+) stays high outside the cell and low inside. This is the main reason sodium is so important and why it is so carefully monitored and scrupulously reabsorbed by the kidneys, but there are plenty more.
Obviously, this is not an accident. Nothing about the way our body functions is an accident, and no matter how well a particular physiological function or mechanism is understood or not, we can be confident that it is as perfect and finely tuned as it can be because each and every bodily function is the result of adaptations and refinements over billions of years of evolution. This is not a typo: I really did mean to write billions of years. Because every single cell of which we are made has evolved from all of its predecessors as far back as the very first organic molecules that eventually organised in the very first cell: a group of more or less self-organising organelles that developed a symbiotic relationship with one another just because it benefitted them in some way, and found it safer to cluster together behind a fatty membrane through which they could interact with the outside on their own terms.
The aim of every single self-organising entity, from the simplest virus, bacterium or organelle like the mitochondria (our cellular energy-production furnaces), to highly specialised cells in the brain, in the liver or lining a part of the microscopic nephron tubule of one of the millions of these specialised filtering units in our kidneys, to largest groupings of cells in tissues, organs and systems of organs, has always been and always will be the same: survival. Therefore, to understand living systems objectively we have to understand them from the fundamental perspective of the cell itself, the tissue, the organ and the system of organs itself because every adaptation it undergoes is always aimed at improving its own odds of survival. It is very important to keep this in mind and know that everything that happens in a living system always does so in relation to something else and always for good reason, even when we don’t understand the reason, which in itself is also very important to remember.
I use this opportunity to whole-heartedly recommend Lewis Dartnell’s book Life in the universe. Almost every page for me was a delightful discovery of things I was unaware of and found the book truly illuminating.
Coming back to salt, even though we look mostly at sodium and chloride that are the principal constituents of any kind of salt we put on our food, I very strongly recommend always and exclusively using a real salt: any kind of unrefined sea salt (French, cold water, Atlantic salt is particularly clean and rich in trace minerals), Himalayan salt, Smart Salt or Real Salt (the last two are registered trade marks and very rich in trace minerals). On the contrary, I strongly discourage eating chemically manufactured table salt or even refined sea salt, which are not only stripped of trace minerals found in natural, unrefined salts, but contain varying amounts of chemical additives such as whitening agents, for instance.

Unrefined sea salt from the Atlantic coast – Sel de Guerande.
Now, without regard for polemical disputes, pseudo-scientific discussions and debates, or otherwise unfounded views and opinions about salt, can we answer the simple question: how much salt should we generally eat? I believe we can, but although it may seem so, it is not that simple a question. So let’s first ask a simpler one:
How do we make a solution with the same concentration of sodium and chloride as our blood plasma?
To answer this our approach is simple: use the mean concentrations of sodium and chloride in the blood to calculate how much salt we need to match these such that drinking our salt water solution will neither increase nor decrease their concentration. It might seem a little technical at first, but bear with me, it is in fact quite simple.
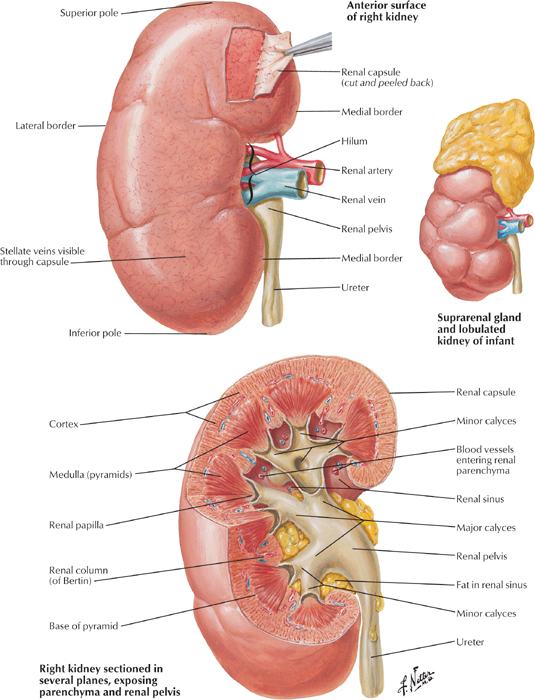
This approach is rather well motivated physiologically because the kidneys’ primary function is to maintain blood pressure and concentration of electrolytes—sodium above all others, and each within its typically narrow range of optimal concentration—while excreting metabolic wastes. The kidneys do this by efficiently reabsorbing most of the water and electrolytes from the large volume of blood that goes through them continuously throughout the day and night, getting rid of as much as possible of the metabolic wastes, and carefully adjusting the elimination of ‘excessive’ amounts of water and electrolytes. (You will soon understand why I placed quotation marks around the word excessive.) Let’s start.
You already know that the mean concentration of sodium in the blood is 140 mmol/l. What we haven’t mentioned is that it must be maintained in the range between 135 to 145 mmol/l. You also know that the mean concentration of chloride is 100 mmol/l, and it must be maintained between 95 and 105 mmol/l. The atomic mass of Na is 23, hence one mole (abbreviated mol) is 23 g, and thus one millimole (abbreviated mmol) is 23 mg. The atomic mass of Cl is 35.5, hence one mole is 35.5 g, and therefore one millimole is 35.5 mg. The molecular mass of NaCl is the sum of the atomic masses of Na and Cl, which implies that one mole of NaCl is 58.5 g, and a millimole is 58.5 mg. (A mole is the amount of substance that contains 6×10^23, Avogadro’s number, elementary entities, in this case, atoms. The molar mass is the same as the atomic or molecular mass.)
Multiplying the concentrations in mmol/l by the molar mass in mg/mmol we get the concentration in mg/l. For Na this equals 140 x 23 = 3220 mg/l or 3.22 g/l, and for Cl it is 100 x 35.5 = 3550 mg/l or 3.55 g/l. This is the mean concentration of sodium and chloride there is in our blood. For a small person like me, weighing, say, 56 kg, there are 4 litres of blood that contain a total of 13 g of Na and 14 g of Cl. This is equivalent to about 2 tablespoons of salt.
It is important to note that this is truly quite a lot in comparison to other ions or molecules in our blood. Glucose, for example, which many—probably most people—mistakenly think as the ‘energy of life’, giving it such great importance, is ideally maintained around 80 mg/dl or 0.8 g/l. This is, therefore, also the amount we would need to add to our salt and water solution to make it have, in addition to that of the salt, the same concentration of glucose as that of our blood. And 0.8 g/l for 4 litres of blood makes a total of 3.2 g of glucose in that (my) entire blood supply. This is about 10 times less than the amount of salt! What does this tell you about their relative importance in our system?
Now, given that Cl (35.5) is heavier than Na (23), NaCl will have a higher mass fraction of Cl: its mass will be 60% chloride (35.5/58.5) and 40% sodium (23/58.5). This just means that 10 g of NaCl or salt has 6 g of Cl and 4 g of Na. So to get 3.22 g of sodium, we need 8 g of sodium chloride, which provides 4.8 g of chloride.
The simple conclusion we draw from this calculation is that dissolving a somewhat heaping teaspoon of salt in one litre of water gives a solution that has the same concentration of sodium as that of our blood (with a little extra chloride).
Does this mean that we should generally drink such a salt and water solution? No, I don’t think so. Are there times when we should? Yes, I believe there are. But say we drink 4 litres per day, 8 g of salt per litre adds up to 32 g of salt just in the water we drink! If we add even half of this amount to our food, we are looking at about 50 g of salt per day! Isn’t this utterly excessive, especially since we are told by the medical authorities to avoid salt as much as possible, with some people today consuming nearly no salt at all? (This article here takes a sobering look at the evidence—actually, the lack thereof—of the claimed benefits of salt reduction.) And more questions arise: What happens when we eat less salt? What happens when we eat more? What happens when we drink less water? What happens when we drink more?
Eating more or less salt. Drinking more or less water.
Remember that the kidneys try very hard to maintain the concentration of solutes in blood plasma—to maintain plasma osmolarity. Also remember that sodium is by far the most important in regulating kidney function, and it is also in the highest concentration. It is nonetheless total osmolarity that the kidneys try to keep constant, and besides sodium, the other important molecule used to monitor and maintain osmolarity by the kidneys is urea—the primary metabolic waste they are trying to eliminate.
As an aside to put things in perspective about the importance of sodium, plasma osmolarity is typically estimated by medical professionals using the sum of twice the concentration of sodium with that of urea and glucose: calculated osmolarity = 2 Na + urea + glucose (all in mmol/l). Since sodium is typically around 140 mmol/l whereas glucose is less than 5 mmol/l and urea about 2.5 mmol/l, it’s obvious that we could just forget about the latter two whose contribution is less than 3% of the total, and look exclusively at sodium concentration (2 Na = 280; glucose + urea = 7.5, so their contribution is 7.5/(280+7.5) = 2.6%).
Eating anything at all, but especially salt or salty foods, raises plasma osmolarity. In response—to maintain constant osmolarity—the kidneys very efficiently reabsorb water and concentrate the urine. Drinking water dilutes the blood and therefore lowers its osmolarity. In response, the kidneys very scrupulously reabsorb solutes and eliminate water, hence diluting the urine.
If we eat nothing and just drink plain water, beyond the body’s minimum water needs, every glass will dilute the blood further and thus cause the kidneys to try to retain more of the sodium while eliminating more of the water. We are drinking quite a lot, but as the day progresses, we are growing more thirsty. We drink more but go to the bathroom more frequently, our urine grows more diluted, and by the end of the day we find ourselves visibly dehydrated, with chapped lips and dry skin. This seems paradoxical in that while drinking water, we are getting increasingly dehydrated. But it is not paradoxical. It is simply the consequence of the kidneys doing their work in trying to maintain constant blood plasma concentrations of sodium (and solutes). For those of you who have fasted on plain water for at least one day, you mostly likely know exactly what I’m talking about. For those who have not, you should try it and experience this first hand for yourselves. Avoiding dehydration in this case is simple: eat salt to match water intake.
If, on the other hand, we do not drink, then the blood gets more and more concentrated, the concentration of sodium and other ions, urea, and everything else for that matter, rises with time, and the kidneys keep trying, harder and harder with time, to maintain the osmolarity constant by retaining as much as they possibly can of the water that is present in the blood. You might think: why not just eliminate some of the solutes to lower their excessively high concentration? But eliminating solutes can only be done through the urine, which means getting rid of water that, in this state of increasing dehydration, is far too precious, and the kidneys therefore try to retain as much of it as possible, hence concentrating the urine as much and for as long as possible to make full use of the scarce amount of water that is available for performing their functions. But here is a crucial point to understand and remember:
In order to reabsorb water, the kidneys rely on a high concentration of solutes—hyperosmolarity—in the interstitial medium through which passes the tubule carrying the filtrate that will eventually be excreted as urine. This is how water can be reabsorbed from the filtrate: the higher the difference in concentration, the more efficient the reabsorption. If there is plenty of excess salt—sodium and chloride ions—then these solutes is what the kidneys prefers to use to drive up and maintain the hyperosmolarity of the interstitial medium, and urea can be excreted freely. If, however, there is a scarcity of sodium and chloride ions, then the kidneys will do everything to reabsorb as much of the precious ions that are in circulation to maintain adequate concentrations of these in the bloodstream, and at the slightest sign of water shortage and dehydration—to ensure the hyperosmolarity of the interstitial medium for maximum water reabsorption—the kidneys will begin to recycle urea, excreting progressively less of it as dehydration increases.
Most of you will have experienced a long day walking around, maybe while on a trip visiting a city, during which you did not drink for several hours. You might have also noticed that you probably didn’t go to the bathroom either, which you may have found unusual compared to the frequency with which you usually go pee when you’re at home or at work. You will have noticed that your mouth was drier and drier as the hours passed, but also that you felt more and more tired, heavy-footed and without energy. Eventually it struck you just how thirsty you were, or you were finally able to find water to drink, and drank to your heart’s content. As you drank, you might have felt a surge of energy within as little as a minute or two or even immediately following the first few sips. Soon after, you finally did go to the bathroom, and noticed how incredibly dark and strong smelling your urine was. Now you understand what was happening in your kidneys, why you didn’t go pee for these long hours, why your urine was so dark and smelled so strong. However, the reason why you felt your energy dwindle as the hours passed, and then return when you drank is still unclear.
Water in the blood regulates its volume. And volume in a closed system determines internal pressure. Our circulatory system is a closed system in the sense that there are no holes where blood either goes in or comes out. Yet at the same time it is not a closed system because water enters and leaves the system: it enters the bloodstream through the wall of the intestines, and leaves it through the kidneys and out into the urine. All physiological functions depend intimately on blood pressure: whether it is shooting up through the roof as we face a huge brown bear towering over us and growling at the top of its lungs, and priming us in this extremely stressful fight-or-flight situation for some kind of high-energy reaction in response, or whether it is as low as it can be during our most soothing and restful sleep deep into the night, when the body is repairing and rebuilding itself. And what is the primary regulator of blood pressure? The kidneys.
I will address the details of how the kidneys function and regulate pressure and osmolarity in another post. For now, what is relevant to understand why your energy faded as the hours passed or, more precisely, as the body got progressively more dehydrated, is straight forward:
As water content decreases, blood volume decreases. As the volume decreases, blood pressure drops. And as blood pressure drops, energy levels go down. It’s as simple as that.
It does not help that as soon as the kidneys detect dehydration and drop in pressure, they release hormones to provoke the contraction of the blood vessels in order to counter the pressure drop. This works to a great extent, but since the arteries and veins are constricted, blood flow throughout the body decreases, which in turn contributes significantly to our feeling increasingly heavy-footed and sleepy. With every passing minute, dehydration increases, pressure decreases, blood vessels contract more and our energy level drops further, to the point where we just want to sit down, or even better, lie down, right here on this park bench, and have a long nap.
Interesting, isn’t it? And here again there is nothing strange or paradoxical in this self-regulating mechanism that eventually puts us to sleep as we get increasingly dehydrated. It is simply the consequence of the kidneys doing their work in trying to maintain constant osmolarity and blood pressure. Avoiding dehydration in this case is even simpler: drink water.
If you’ve read this far, you know that both solutions to prevent dehydration are intimately linked: if we don’t drink enough water we get dehydrated, but if we drink too much water without eating salt we also get dehydrated. So let’s now ask another question:
Precisely how much water?
An adult human being needs on average a minimum of 3 litres of water per day to survive for more than a few days (Ref). This depends on climate and level of activity and a bunch of other factors, but in general the range is well established to be between 2 litres in cooler and 5 litres per day in the hottest climates. As suggested from our previous considerations, minimum water intake is also related to salt and food intake. And although this was obvious to me from my own experience of fasting rather regularly between 1 and 3 days at a time, I had not read about it. But as it turns out, the NRC and NAS both (independently) estimated minimum water intake as a function of food intake to be between 1 and 1.5 ml per calorie. For a diet of 2000 calories this would amount to between 2 and 3 litres. But this obviously does not mean that if we don’t eat anything, we don’t need any water! So, what is the very strict minimum amount of water the body needs before physiological functions break down? The short answer is 1.1 litres. For the slightly longer answer, here is a excerpt from page 45 of The Biology of Human Survival:
If obligatory losses are reduced to an absolute minimum and added up, the amounts are 600 milliliters of urine, 400 milliliters of insensible skin loss, and 200 milliliters of respiratory water loss, a total of 1.2 liters. Because maximum urine osmolarity is 1200 milliosmoles/liter, if diet is adjusted to provide the minimum solute excretion per day (about 600 mOsmol), minimum urine output may fall, in theory, to 500 milliliters per day and maitain solute balance. Hence, the absolute minimum water intake amounts to just more than 1 liter (1.1) per day.
(This is also taught in renal physiology lectures such as this one. If you are interested, you will learn a lot from this longer series of 13 segments on urine concentration and dilution here, as well as from this series of 7 segments on the renin-angiotension-aldosterone system here. I found all of them very instructive.)
Keep in mind that 1100 ml of water per day is the very bare minimum for survival, and that there are absolutely no other water losses: basically, you have to be lying, perfectly calm and unmoving at an ideal room temperature where you are neither hot nor cold, not even in the slightest. That’s not particularly realistic unless you’re in a coma. And to show just how extreme it is, let’s see how much of the water the kidneys need to reabsorb to make this happen:
For someone like me weighing 57 kg, the mass of blood is 57*7% = 4 kg. Since the density is almost equal to that of water, 4 kg corresponds to 4 litres. Of this, we know that plasma accounts for a little more than half (54.7%) by volume which makes 2.2 litres, and since plasma is 92% water, the volume of free water in the blood supply is almost exactly half: 2 litres. Blood flow through the kidneys is, on average, around 1.2 l/min. This amounts to more than 1700 litres per day, and means that for 4 litres of blood in the body, every drop of blood goes through the kidneys 425 times in 24 hours, each and every day.
In the kidneys the first step in filtration is the “mechanical”, particle-size-based separation of the blood’s solids from its liquid component. Water makes up half the blood volume, and therefore represents half the flow through the kidneys: 0.6 l or 600 ml/min (850 litres per day). But only 20% of the total flow goes through nephron filtration, which makes 120 ml/min. In the extreme case we are considering, urine output is taken to be 500 ml in 24 hours, equivalent to 20.83 ml/hour or 0.35 ml/min (500 ml/24 h/60 min). Therefore, to achieve this, the kidneys must reabsorb 119.65 ml of the 120 ml flowing through them every minute. This translates to an astounding 99.7% reabsorption efficiency! I’m very skeptical that your average person’s (generally compromised) kidneys could achieve this, but the point was to quantify how extreme this situation at the limit of human survival really is, and as you can see, it is indeed as extreme can be.
Also, keeping in mind that these minimum vital physiological water losses in these circumstances would occur at a more or less uniform rate throughout the day, it would probably be much better to drink a little at regular intervals during our walking hours than to drink everything at once and nothing else during the remaining 24 hours. But what would be the ideal rate at which we should replenish our water in these extreme circumstances?
Assuming the theoretically minimum combined water losses of 1100 ml are lost evenly over the course of the 24 hours, this corresponds to a water loss rate of 0.76 ml/min (1100 ml/24 h/60 min). This is therefore the ideal rate at which to replenishing it. In practice, we may not have an IV system to do this for us, and we will probably be sleeping long nights as our heart rate and blood pressure will have hit rock bottom. Drinking 1100 ml in 11 hours (to work with round numbers) could be done by taking 100 ml, (half a small glass), every hour. This would be the simplest and most reasonable way to maintain solute balance as best we can.
Naturally, with such a minimal water intake, the kidneys are struggling to maintain osmolarity by retaining as much water as possible. Any additional intake of salt (or food) would make things worse in the sense that it would raise the concentration of sodium (and solutes) in the blood whose balance the kidneys will not be able to maintain without additional water. But remember that eating a 200 g cucumber, for example, supplies nearly no calories as it contains virtually no sugar, fat or protein, while proving almost 200 g (ml) of water. And that, conversely, any drink containing caffeine or alcohol will actually dehydrate as those substances are diuretic and cause the excretion of free water.
A somewhat more realistic scenario is one in which we are not eating, but very moderately active at comfortable temperatures. In this case, most experts would agree that the minimum water requirements would be around 2 litres per day. Since we are fasting, these additional water needs are due to greater water losses through evaporation and physiological activity; not to offsetting increased water needs due to food consumption. Consequently, we should ideally drink about 10 glasses of 200 ml, one approximately every hour from 7h to 19h, and we should not eat any salt.
More realistic but still not so common, is that you are doing a 24 hour fast. The purpose of the fast is to give a break to the digestive system, rehydrate bodily tissues, stimulate more fat burning and flush toxins out of the system. Say we drink 4 litres instead of the minimum of 2. In this case we should, in fact, eat some salt in order to ensure good hydration of tissues by supplying plenty of water through a well hydrated bloodstream without diluting the sodium and thus causing the kidneys to excrete more water. And this brings us back to the basic question that set us on this rather long investigation:
Precisely how much salt?
But you already know the answer to this question: 1 teaspoon per litre in 2 of the 4 litres. Because we don’t drink during the night for about 12 hours, the body inevitably gets dehydrated. Therefore, the best strategy is to start with plain water to rehydrate the concentrated blood and bodily tissues dehydrated from the night, and end with a litre of plain water in preparation for the dry night coming. You should take the equivalent of 1 generous teaspoon of salt with each of the additional litres of water during the day. This will ensure proper hydration of tissues by preventing excessive dilution of blood sodium levels, and maximum urea excretion. Excess sodium, chloride and any other electrolyte will be readily excreted in the urine.
Finally, the far more realistic scenario and, in fact, the one that for most of us is the everyday, is that we are normally active and eating around 2000 calories a day, typically over the course of about 12 hours. In this case we need the basic 2 litres to offset minimum evaporation and physiological losses, and between 2 and 3 litres to offset the 2000 calories. This makes between 4 and 5 litres, 2 of which must be plain water, and 2 or 3 of which must be matched by a good teaspoon of salt per litre that will most naturally, and maybe also preferably, be taken with the food.
Keep in mind that this is the total salt requirements and many prepared foods contain quite a lot already. The hotter or drier the climate, the more water we need. The more we exercise, the more water and the more salt we need. The more we sweat, the more water and the more salt we need. The more stress we experience, the more water and the more salt we need. And in all of these cases, we also need a lot more magnesium.
By the way, it is interesting but not surprising that this conclusion on the amount of salt per day: about 10-15 g, is also the recommendation of the late Dr Batmanghelidj, the “Water doctor”, as well as that of Drs Volek and Phinney, the “Low-Carb doctors” (see References for details), although the former emphasises the importance of an abundant water intake, while the latter hardly mention it if at all.
So this is it. We know how much water we should generally drink, and we know how much salt we should generally eat:
We should always drink the bare minimum of 2 litres per day. Ideally we should drink 4-5 litres every day. If for some reason we drink 2 litres or less, we should not take any salt (or food for that matter!). If we drink more than 2 litres, we should match each additional litre of water with 1 teaspoon of salt, taking into account the salt contained in the food we eat. It is always better physiologically to drink more than to drink less. And remember that we hydrate most effectively on an empty stomach by drinking 30 minutes before meals.
40.416775
-3.703790